
I still remember the first time a patient walked into my clinic complaining of persistent bone pain and unexplained fatigue. She lived in Dubai, enjoyed year-round sunshine, and assumed her lifestyle protected her from any nutritional deficiencies. Her blood tests told a different story.
Her Vitamin D levels were dangerously low.
This scenario plays out in my clinic almost every week. Despite the UAE’s abundant sunshine, Vitamin D deficiency has become one of the most underdiagnosed health conditions affecting our population. Studies suggest that up to 90% of UAE residents may have insufficient Vitamin D levels, with women being particularly vulnerable.
What makes this situation so puzzling is the irony: we live in one of the sunniest places on Earth, yet we are suffering from a deficiency that sunlight should naturally prevent. The reasons are deeply rooted in our modern lifestyle choices, from air-conditioned offices that keep us indoors during peak sun hours to the tinted windows that block UV rays from reaching our skin.
In this article, I want to share what I have learned about the critical connection between Vitamin D deficiency and musculoskeletal health. I will walk you through the warning signs, the real risks to your bones and joints, and most importantly, what you can do to protect yourself and your family. If any of this resonates with you, I encourage you to book a routine screening at our hospital. A simple blood test could be the first step toward feeling like yourself again.
Before we dive into the symptoms and health impacts, let us take a moment to understand what Vitamin D actually is and why it matters so much for your body.
Vitamin D is technically not a vitamin at all. It is a hormone that your body produces when your skin exposed to ultraviolet B rays from sunlight. This hormone then travels through your bloodstream to your liver and kidneys, where it gets converted into calcitriol, the active form that your body can use.
Think of Vitamin D as the key that unlocks your body’s ability to absorb calcium from your food. Without enough Vitamin D, no matter how much calcium you consume through your diet or supplements, your body simply cannot utilize it effectively. This is why Vitamin D deficiency directly translates to calcium deficiency in practical terms, even when your dietary calcium intake is adequate.
The sunshine vitamin, as some call it, plays several crucial roles in your body. It maintains strong bones by helping your intestines absorb calcium and by regulating the minerals in your blood that keep your bones healthy. It supports your immune system, helping you fight off infections. It influences your mood and mental health. And importantly for this discussion, it is essential for proper muscle function and nerve communication between your brain and body.
When you do not have enough Vitamin D circulating in your system, these fundamental processes start to break down, often in ways that creep up gradually and get misattributed to aging, stress, or other conditions.
The UAE presents a fascinating paradox when it comes to Vitamin D. We have sunshine available every single day of the year, yet we have become one of the most Vitamin D deficient populations in the world. Understanding why requires us to examine our cultural and lifestyle patterns.
The primary culprit is our indoor lifestyle. In a country where summer temperatures regularly exceed 45 degrees Celsius, spending time outdoors during the day feels impractical at best and dangerous at worst. Our lives are organized around air-conditioned spaces: homes, offices, shopping malls, cars. We wake up indoors, commute in air-conditioned vehicles, work in sealed buildings, and return home without ever having meaningful sun exposure.
Tinted windows contribute to this problem in ways we rarely consider. Our cars have tinted windows, our homes have tinted windows, our offices have tinted windows. Even when we are outdoors, the UV rays that our skin needs to produce Vitamin D are being filtered out before they can reach us.
Our traditional clothing choices also play a role. The flowing abayas and traditional dress that are comfortable and culturally appropriate in the heat also cover most of our skin, preventing sun absorption. While this is not a reason to change cultural practices, it is an important factor to recognize when assessing our Vitamin D risk.
Another factor is our predominantly indoor social life. Unlike in countries where people spend time in parks, gardens, or outdoor cafes year-round, our socialization happens in air-conditioned spaces. Children play indoors in malls rather than in parks. Young professionals exercise in gyms rather than outside. Families gather on rooftop terraces only in the cooler months.
The result is a population with minimal cumulative sun exposure despite living in a desert with endless sunshine. Most of us get our necessary UV exposure in brief moments: walking from a parking garage to an office, or during the early morning or late evening when we might step outside. This is rarely enough to maintain healthy Vitamin D levels.
Now let us get to the heart of the matter: how does low Vitamin D actually cause joint pain and musculoskeletal discomfort?
The connection operates through several mechanisms that I will explain in practical terms.
First, Vitamin D directly influences bone metabolism. Your bones are not static structures. They are constantly being broken down and rebuilt in a process called bone remodeling. Vitamin D helps regulate this process by controlling calcium absorption and by directly acting on bone-forming cells called osteoblasts. When Vitamin D is insufficient, this balance tips toward bone loss rather than bone building, leading to weakened bone structure that can manifest as pain.
Second, Vitamin D is crucial for muscle function. Your muscles have Vitamin D receptors on their surfaces, and when this hormone binds to these receptors, it helps maintain muscle strength and function. In my clinical experience, many patients with low Vitamin D complain of generalized muscle weakness, particularly in the large muscle groups of the thighs and upper arms. This muscle weakness puts additional strain on joints, which then ache and feel uncomfortable.
Third, Vitamin D has anti-inflammatory properties. Research has shown that Vitamin D helps modulate the immune response and can reduce inflammatory markers in the body. Without adequate Vitamin D, inflammation in joint tissues may increase, contributing to pain and discomfort that patients often describe as diffuse or widespread.
Fourth, nerve function depends on Vitamin D. The numbness, tingling, and burning sensations that many Vitamin D deficient patients describe are related to how Vitamin D affects nerve growth and function. When your nerves are not receiving the signals they need due to low calcium levels caused by Vitamin D deficiency, they can misfire, sending pain signals that feel like they are coming from your joints.
This is why many patients describe their joint pain as a deep, aching sensation that does not match any specific injury or activity. It is a systemic issue, not a localized problem.
One of the most common complaints I hear from patients with Vitamin D deficiency is exhaustion. They describe a fatigue that sleep does not fix, a tiredness that persists no matter how much they rest.
This connection is not imaginary. Research has consistently shown that Vitamin D plays a vital role in energy production and muscle function, both of which directly impact how energized you feel throughout the day.
When your muscles are weak from Vitamin D deficiency, every physical activity requires more effort. Climbing stairs, carrying groceries, even walking through the mall becomes harder than it should be. Your body expends more energy to accomplish the same tasks, leaving you feeling depleted.
Additionally, Vitamin D is involved in mitochondrial function. Your mitochondria are the powerhouses of your cells, converting food into usable energy. When Vitamin D levels are low, this energy production process becomes less efficient, contributing to the profound fatigue that characterizes this deficiency.
Many patients also report cognitive symptoms alongside their physical fatigue. They describe brain fog, difficulty concentrating, and memory problems. This makes sense given that Vitamin D receptors are present throughout the brain, particularly in areas involved in mood and cognition.
In the UAE context, I have noticed that this fatigue often gets attributed to the heat, to busy lifestyles, or to stress. While these factors certainly contribute, dismissing persistent fatigue without checking Vitamin D levels means missing a treatable cause that could dramatically improve quality of life.
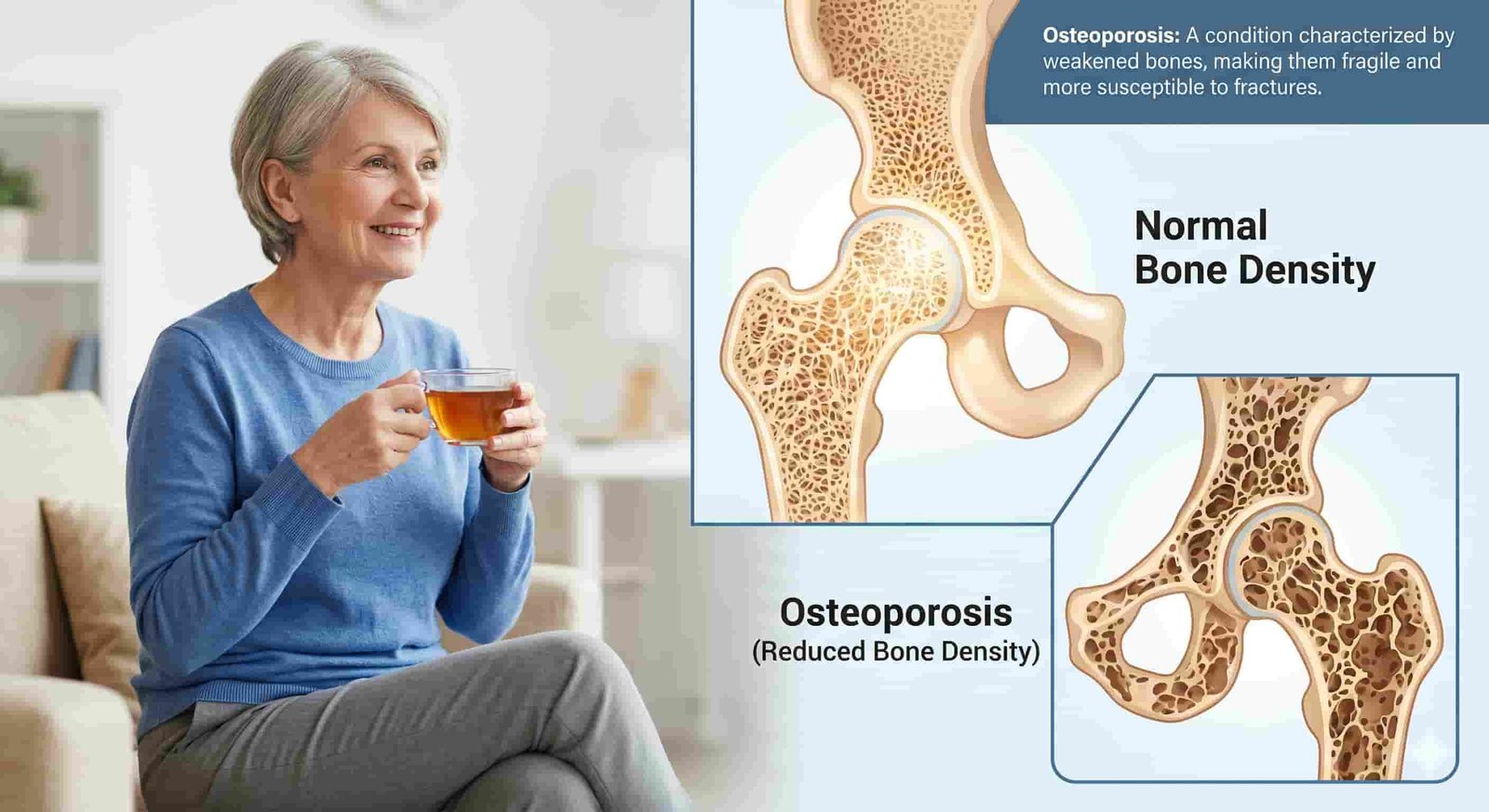
If joint pain and fatigue were not concerning enough, the relationship between Vitamin D deficiency and osteoporosis deserves serious attention.
Osteoporosis is a condition where your bones become porous and fragile, making them susceptible to fractures from minor trauma. What makes it particularly dangerous is that it often develops silently, without obvious symptoms, until a fracture occurs. It is called the silent disease for good reason.
The connection to Vitamin D is straightforward but critical. Without sufficient Vitamin D, your body can only absorb about 10 to 15 percent of the calcium you consume. With adequate Vitamin D, this absorption jumps to 30 to 40 percent. This dramatic difference means that even if you are drinking milk, eating cheese, and taking calcium supplements, your bones may still be starved for the calcium they need if your Vitamin D is low.
Over time, this chronic calcium deficiency causes bone loss. Your body begins removing calcium from your bones to maintain necessary blood levels for heart, muscle, and nerve function. The result is progressively weaker bones that may not give any warning signs until they break.
For women in the UAE, this risk is especially significant. Several factors converge to increase osteoporosis risk: lower baseline Vitamin D levels than men, reduced sun exposure due to cultural practices, high rates of veiling, and for post-menopausal women, the loss of estrogen’s bone-protective effects.
A bone density scan can detect osteoporosis before fractures occur, allowing for early intervention. This scan is painless, non-invasive, and takes only minutes. Given the prevalence of Vitamin D deficiency in our population, I consider it an essential screening tool for anyone over 50, and for younger individuals with risk factors.
Based on my clinical experience and supported by medical research, here are the common signs that may indicate Vitamin D deficiency.

Women in the UAE face compounded risks when it comes to Vitamin D deficiency, and I want to address this specifically.
The physiological reasons for increased vulnerability start early. Adolescent girls and young women who avoid sun exposure for aesthetic reasons or due to busy lifestyles are building weaker bone banks that they will draw from throughout their lives. Peak bone mass is achieved in the late twenties, and what you build then protects you in your later years.
During reproductive years, heavy menstrual bleeding can contribute to iron deficiency, which can compound fatigue from Vitamin D deficiency. Pregnancy and breastfeeding further deplete maternal nutrients, including Vitamin D, making adequate repletion essential for both mother and developing baby.
The cultural factors I mentioned earlier, particularly extensive skin coverage and indoor lifestyles, affect women disproportionately due to garment choices. This is not a criticism of cultural practices, but rather an acknowledgment of a medical reality that requires proactive management.
Post-menopause, the stakes become even higher. Estrogen provides significant bone protection, and when it declines during menopause, bone loss accelerates. Without adequate Vitamin D to maximize calcium absorption, postmenopausal women face exponentially higher osteoporosis risks.
For women experiencing symptoms like hair loss, fatigue, or bone pain, I strongly recommend including Vitamin D testing as part of any health evaluation. The normal range for women is the same as for men, but the interpretation may differ based on reproductive status and age.
Understanding Vitamin D test results requires knowing what numbers to aim for and what they mean clinically.
The standard blood test for Vitamin D is called the 25-hydroxyvitamin D test, often abbreviated as 25(OH)D. Results are typically reported in nanograms per milliliter (ng/mL) or nanomoles per liter (nmol/L).
I should mention that there is some debate about ideal target levels, and your doctor may have specific recommendations based on your individual health profile. Additionally, extremely high Vitamin D levels can be harmful, so more is not always better. This is why testing and medical guidance are essential rather than self-prescribing high-dose supplements.
Getting tested for Vitamin D deficiency is straightforward and requires only a simple blood draw.
The test itself is affordable, and many patients are surprised to learn that Vitamin D testing is now considered routine rather than specialized. The process involves no fasting, no special preparation, and minimal discomfort. Your blood sample is sent to a laboratory, and results are typically available within 24 to 48 hours.
What I want patients to understand is that this test is not just about getting a number. It is about establishing a baseline so we can create an appropriate treatment plan. If you are deficient, we will recommend supplementation at a specific dose based on your level of deficiency. We will then retest after a few months to ensure levels are rising appropriately and to adjust dosing if needed.
A bone density scan, or DXA scan, provides additional information about your skeletal health. This scan measures bone mineral density at the hip and spine, the two sites most susceptible to osteoporotic fractures. It is recommended for all women over 65, all men over 70, and younger individuals with risk factors such as family history of osteoporosis, smoking, excessive alcohol use, long-term steroid use, or history of fractures.
At our hospital, we offer comprehensive bone health assessments that combine Vitamin D testing with bone density scanning, giving us a complete picture of your skeletal wellbeing. I believe this approach is essential for our patient population given the high prevalence of deficiency.
The good news about Vitamin D deficiency is that it is treatable, often with excellent results.
For those with osteoporosis or high fracture risk, prescription-strength Vitamin D may be recommended, sometimes combined with calcium supplements. This is particularly important for postmenopausal women and older adults.
Lifestyle modifications can support treatment. Regular weight-bearing exercise strengthens bones. Quitting smoking and limiting alcohol support bone health. Ensuring adequate dietary calcium is also important, though many patients are surprised to learn that calcium should not be taken at the same time as Vitamin D supplements, as they compete for absorption.
I want to be clear about when self-care is sufficient and when professional evaluation is necessary.
You should schedule an appointment with your doctor if you are experiencing any of the symptoms I have described, particularly persistent bone or muscle pain, unexplained fatigue, or frequent infections. You should also be tested if you are at high risk for deficiency due to limited sun exposure, have malabsorption syndromes, are taking medications that affect Vitamin D metabolism such as certain seizure medications, or have a history of osteoporosis in your family.
If you are over 50 and have never had a bone density scan, or if you are a postmenopausal woman concerned about bone health, a comprehensive evaluation including Vitamin D testing and bone density assessment would be appropriate.
I also recommend testing for anyone planning pregnancy, as adequate Vitamin D is important for fetal bone development and maternal health during pregnancy and breastfeeding.
Understanding your Vitamin D status is one of the most valuable steps you can take for your long-term health.
You may choose to get your Vitamin D levels tested and, if needed, undergo a bone density scan at a trusted healthcare facility. A qualified medical professional can interpret your results in the context of your overall health, lifestyle, and risk factors, and guide you with a personalized plan to support your bone strength.
The process is simple. Most clinics and hospitals offer Vitamin D blood testing without any special preparation. Results are typically available within a couple of days, after which a doctor can review them with you and recommend appropriate next steps.
If you are experiencing persistent bone pain, muscle weakness, or unusual fatigue that lasts for more than 5–7 days, it is important to consult a nearby hospital or healthcare provider for proper evaluation.
Do not wait until a fracture to discover weakened bones. Do not assume that ongoing fatigue is just part of a busy life. These symptoms often have underlying causes, and Vitamin D deficiency can be one of them.
Your bones support you every day. Taking timely steps now can help keep them strong and healthy for years to come.
For those in Dubai, Health Call Clinic offers rheumatology services, including Vitamin D testing and consultations with experienced rheumatologists.
How much sun exposure do I need to maintain healthy Vitamin D levels?
In the UAE context, aim for about 10 to 15 minutes of sun exposure on uncovered arms and legs each day, ideally before 10 AM or after 4 PM to minimize UV intensity. However, this alone may not be sufficient for everyone, which is why testing is important.
Can I get enough Vitamin D through diet alone?
It is very difficult to get adequate Vitamin D from food. You would need to eat fatty fish daily or consume large amounts of fortified foods to approach recommended levels. Most people need some supplementation, especially during months of heavy indoor living.
How long does it take to correct Vitamin D deficiency?
With appropriate supplementation, Vitamin D levels typically begin to rise within four to six weeks. However, replenishing your body’s stores completely may take several months. Retesting after about three months of treatment is standard practice to ensure progress.
Are there any side effects from Vitamin D supplements?
When taken as directed by your doctor, Vitamin D supplements are generally safe. However, excessive Vitamin D can cause dangerous calcium buildup, leading to kidney problems. This is why testing and medical guidance are important rather than self-prescribing high doses.
Does Vitamin D deficiency cause hair loss?
Hair loss has many causes, and Vitamin D deficiency is one of them. If you are experiencing hair loss, having your Vitamin D levels checked is a reasonable part of the evaluation. Addressing deficiency may help, though results vary depending on the underlying cause.
Can Vitamin D deficiency cause headaches?
Research suggests that low Vitamin D levels may be associated with tension headaches and migraines. While not everyone with headaches has Vitamin D deficiency, it is a modifiable risk factor worth investigating, especially if headaches are frequent or severe.
Is Vitamin D testing covered by insurance?
Coverage varies by insurance plan and provider. Many basic health insurance plans now include Vitamin D testing as part of routine preventive care. We can help you understand your coverage when you book an appointment.
Vitamin D deficiency is a hidden epidemic affecting hundreds of thousands of UAE residents, silently compromising bone health and contributing to joint pain, muscle weakness, and chronic fatigue. Despite our year-round sunshine, our indoor lifestyles, tinted windows, and avoidance of summer heat mean that many of us are not getting the sun exposure our bodies need.
The connection between adequate Vitamin D and musculoskeletal health is well-established in medical literature. From bone metabolism to muscle function to nerve communication, this sunshine hormone touches every aspect of how we move, feel, and function.
The encouraging message is that Vitamin D deficiency is detectable, treatable, and preventable. A simple blood test can reveal whether you are deficient. Appropriate supplementation, combined with sensible sun exposure and dietary changes, can restore your levels and improve your symptoms.
If you are experiencing any of the symptoms I have described, or if you have risk factors for deficiency or bone disease, I encourage you to book a routine screening at our hospital. Your bones and joints will thank you for years to come.
To schedule a Vitamin D test or bone density scan, contact our clinic or book an appointment through our website today.

Dr. Bassel Darwish
Consultant Rheumatologist.
Medical Director, Health Call Clinic, Dubai Health Care City.
Diplomate, American Board of Rheumatology.
Diplomate, American Board of Internal Medicine.
Fellow, American College of Rheumatology.
Member, American College of Physicians.
Home » How Vitamin D Deficiency Impacts Your Joints and Bones
WhatsApp us